Minor Surgery / Treatment
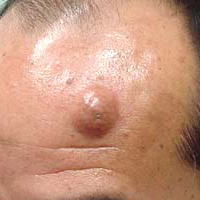
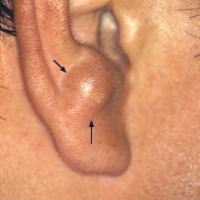
Sebaceous Cyst
A sebaceous cyst is a type of closed cyst that lies below the skin's surface. This kind of cyst fills with a fatty material called sebum (which has been produced by the sebaceous glands in the epidermis). Some consider a sebaceous cyst to be defined not by the sebum content, but rather by the origin being the sebaceous glands. Also, some consider the epidermoid cyst to be equal or at least similar to the sebaceous cyst.
Causes
Some potential sebaceous cyst causes include the following items (may include rare medical causes):
* Basal cell nevus syndrome
* Blocked sebaceous glands
* Dermatobia hominis
* Excessive production of testosterone
* Gardner's syndrome
* Swollen hair follicles
Treatment
After the diagnosis has taken place, a treatment method may begin. Sebaceous cyst treatment options include both surgical and non-surgical. If the cyst has already become infected, it may require additional treatment (such as antibiotics). The patient should not attempt to break or pop the cyst, as infection could occur in the nearby tissue.
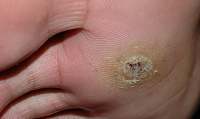
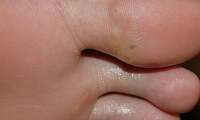
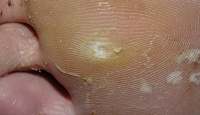
Corns
Corns and calluses can be treated with many types of medicated products to chemically pare down the thickened, dead skin. These products are share the same active ingredient -- salicylic acid, the ingredient used in over-the-counter wart-removal products. Salicylic acid is a keratolytic, which means it dissolves the protein (keratin) that makes up most of both your corn and the thick layer of dead skin which often tops it. Used as indicated on the package directions, these products are gentle and safe for most people.
You should not attempt to cut or shave away corns and calluses at home. This can lead to potentially dangerous infection of the surrounding tissues. This should be performed by a podiatrist or other health-care practitioner.
If the corn bothers you and doesn't respond to salicylic acid and trimming, you might consider seeing a physician who can physically pare corns with scalpels.
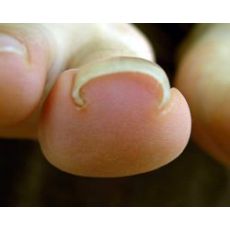
Ingrown Nail
Having an ingrown toenail can be extremely painful. An ingrown toenail can make walking very uncomfortable and lead to infection. Most often an ingrown toenail develops because a person trims the corners of their toenails down too far. A lot of people like to cut their toenails in a rounded off shape but this can cause the toenails to grow into the sides of the skin when it starts to grow back. Although this can happen on any of the toes, it is most commonly found on the big toe. Also wearing tight fitting shoes can cause this to happen.
Ingrown toenail treatment
If you are beyond self treatment because an infection has started to set in then you need to see your doctor as soon as possible. In the case of a minor infection your doctor may be able to prescribe some antibiotics and bandage the toe properly so that the toenail is not pressing on the skin. However if the toenail is causing extreme pain and the swelling and infection are really bad, the doctor may have to perform surgery on the toe to remedy the situation. This could mean having some or all of the toenail or surrounding skin cut and removed.
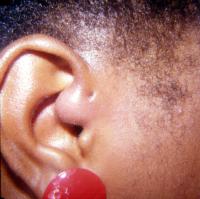
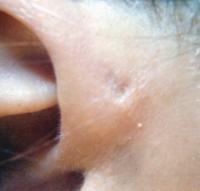
Preauricular sinus (sinus)
Preauricular sinus are common congenital malformations first described by Heusinger in 1864. Preauricular sinus are frequently noted on routine physical examination as small dells adjacent to the external ear, usually at the anterior margin of the ascending limb of the helix. However, preauricular sinus have been reported to occur along the lateral surface of the helicine crus and the superior posterior margin of the helix, the tragus, or the lobule. Anatomically, preauricular sinus are lateral and superior to the facial nerve and the parotid gland.
Surgical Care
Once infection occurs, the likelihood of recurrent acute exacerbations is high, and the sinus tract should be surgically removed.Surgery should take place once the infection has been treated with antibiotics and the inflammation has had time to subside. Controversy regarding indications for surgery exists. Some believe that the sinus tract should be surgically extirpated in patients who are asymptomatic because the onset of symptoms and subsequent infection cause scarring, which may lead to incomplete removal of the sinus tract and postoperative recurrences. The recurrence rate after surgery is 13-42% in smaller studies and 21% in one large study.
Most postoperative recurrences occur because of incomplete removal of the sinus tract. One way to prevent incomplete removal is to properly delineate the tract during surgery. Some surgeons cannulate the orifice and inject methylene blue dye into the tract 3 days prior to surgery under sterile conditions. The opening is then closed with a purse-string suture. This technique distends the tract and its extensions by its own secretion stained with methylene blue.
During surgery, some surgeons use either a probe or an injection of methylene blue dye for cannulation of the orifice. The most successful method is to use both modalities to delineate the entire tract.
Disclaimer:The information contained in this website is provided by HK Specialists Centre for general information and reference only. All information are not guaranteed or warranted to be absolutely accurate and updated. Our centre is not responsible for any losses or damages incurred as a result of the use of the information on this website. HK Specialists Centre is entitled to edit all information on this site at any time at its absolute discretion without giving any reasons.





